Article
Mar 14, 2026
Everything about Perianal Fissure [and treatments]
The perianal fissure is one of the most common causes of persistent anal pain, but many still hesitate to seek medical help. See here for treatments!

An anal fissure is one of the most common causes of persistent anal pain, significantly affecting the quality of life and well-being. Although many people hesitate to seek medical help out of shame or embarrassment, this is a condition that requires careful clinical attention.
It is estimated that up to 20% of patients seeking proctologic care present with anal fissure or perianal fissure, according to data from the American Society of Colon and Rectal Surgeons (ASCRS). Despite being frequent, the diagnosis is still underreported, which contributes to chronic and difficult-to-heal cases.
In today’s article, you will understand what a perianal fissure is, what its symptoms are, the most common causes, and how scientific advances and clinical research are opening new perspectives for those living with this condition.
What is a perianal fissure?
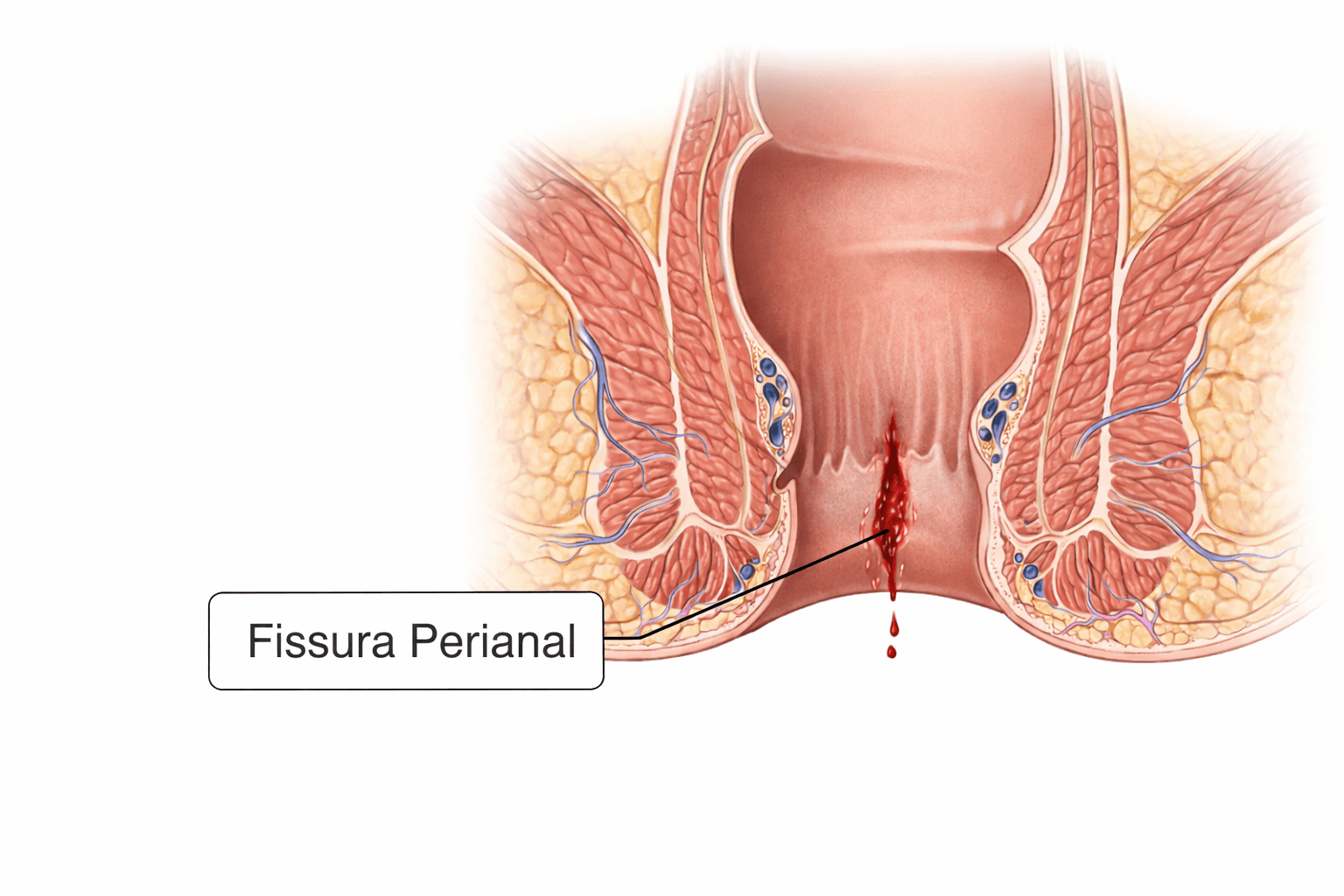
A perianal fissure is a linear or oval wound located in the mucosa lining the anal canal or the skin around the anus. It occurs due to a rupture of the tissue, usually caused by painful bowel movements or severe constipation, creating tension in the anal sphincter and micro-lesions.
Although the term “anal fissure” is often used synonymously, the perianal fissure tends to encompass a slightly larger area - also affecting the skin around the anus (perianal), and not just the internal mucosa.
The MSD Manual describes the condition as a laceration that causes severe pain during and after bowel movements, often accompanied by light bleeding.
The fissure can be acute, when it has been present for less than six weeks and tends to heal with clinical treatment, or chronic, when it persists beyond this period, forming hardened edges and a small fold of skin called papule or sentinel tag.
What are the symptoms of anal fissure?
The symptoms of an anal fissure are markedly painful, which leads many patients to postpone bowel movements for fear of pain - further aggravating the difficulties faced.
The clinical picture includes acute pain during or after bowel movements, presence of bright red blood on toilet paper or in stool, itching, irritation, and involuntary muscle spasms.
The pain tends to be described as a sharp, burning, or deep stabbing sensation, lasting from minutes to hours after defecation.
According to the Cleveland Clinic, this pain can last from minutes to several hours and, in some cases, is associated with involuntary spasms of the internal anal sphincter, which hinder healing and prolong discomfort.
How to tell if it’s an anal fissure or hemorrhoids?
Differentiating anal fissures from hemorrhoids is very important because both can cause pain and bleeding. While hemorrhoids are venous dilations, fissures are linear wounds in the mucosa.
The pain from the fissure is sharp and intense, typically during bowel movements, while hemorrhoidal pain is often superficial and felt as a persistent pressure or itching. Additionally, fissures tend to cause spasms and bleeding in a thin stream, not voluminous.
How to tell if it’s a chronic perianal fissure?
A chronic fissure is characterized by the persistence of symptoms for more than six weeks. In these cases, hardened edges, exposure of muscle fibers, and the presence of small thickened skin near the lesion are observed.
According to the National Institutes of Health (NIH), chronic fissures may be associated with persistent sphincter hypertonia, which reduces local blood flow and impedes healing.
Hence the importance of early diagnosis, as the longer the fissure remains open, the greater the risk of local infection and the formation of secondary fistulas.
What does a fissure in the rectum feel like?
The sensation caused by a perianal fissure is often described with a very specific sensory quality: a sharp and localized pain triggered by passing stool and by the movement of the sphincter, followed by residual pain that can last from minutes to hours.
Besides the pain, the presence of bright red blood and local burning are common. These symptoms have functional expression - avoidance of bowel movements, anxiety, impairment of daily activities, and impact on sexual intimacy.
Among the main complaints found in clinical reports, we can cite:
“Stabbing” pain during bowel movements;
Residual pain for up to an hour or more after defecating;
Visible bleeding on toilet paper;
Sensation of tearing, burning, and perianal itching;
Difficulty sitting and impact on intimate relationships.
The intensity of these symptoms can vary according to the depth of the fissure and the time of evolution. Early diagnosis is necessary to avoid the progression of pain and the risk of chronicity.
What can cause a perianal fissure?
The perianal fissure has a multifactorial etiology (the study of causes and origins), but the main triggering mechanism is mechanical trauma caused by hard stool or excess volume in the anal canal.
This trauma causes rupture in the mucosa, initiating an inflammatory and pain process. If there is no treatment, the spasms of the internal anal sphincter and local ischemia hinder the healing of the wound.
Other factors also contribute to the occurrence and maintenance of the fissure: episodes of diarrhea, inflammatory bowel diseases, vaginal delivery, repeated anal sex, poor diet, and anatomical predisposition in the anal region.
Risk factors for perianal fissure

Before the list, it is important to remember that the physiology of the pelvic floor and bowel habits play a central role in the risk of fissures. Among the main risk factors, we can list:
Chronic constipation and straining.
Low-fiber diet and low fluid intake.
Recurrent diarrhea (irritates and weakens mucosa).
Prolonged/traumatic vaginal delivery.
Inflammatory bowel disease (e.g., Crohn's).
Unprotected anal sex/repeated local manipulation.
After identifying the factors, adjusting dietary habits and specialized follow-up are essential to prevent recurrences.
Possible complications of anal fissures
The truth is that even a simple perianal wound, if not well treated, can evolve into more serious complications. Among the main complications, we can list:
Chronic fissure: with thickened edges.
Formation of fistulas or abscesses: due to local infection.
Persistent spasm of the internal anal sphincter.
Psychological impact: anxiety and fear of defecating.
These complications can severely reduce quality of life and hinder the response to conservative treatments, justifying the importance of clinical studies and new therapeutic approaches.
How is the diagnosis of perianal fissure made?

The diagnosis is predominantly clinical and performed by a proctologist. The physical examination is generally sufficient, although pain can significantly hinder the evaluation.
In chronic cases, the health professional responsible for your care may request a anoscopy or endoscopy to rule out associated diseases, such as Crohn's or anorectal infections.
How to treat perianal fissure?
Treatment for perianal fissure depends on the severity and the time of evolution of the lesion. The goal is to interrupt the pain cycle, reduce spasm, and promote healing.
Continue reading to learn about some treatment options and discover how they work.
Medications
Before listing the recommended medications to treat perianal fissure, it is necessary to emphasize that medication treatment is only the first line in acute fissures, according to the Cleveland Clinic.
The main classes include:
Topical ointments with local anesthetics: relieve pain during bowel movements;
Topical sphincter relaxants: reduce anal pressure and promote healing;
Laxatives and dietary fibers: soften stool and prevent new lacerations.
After consistent use and medical guidance, many acute cases heal without the need for surgery.
Surgery
Surgery, known as internal lateral sphincterotomy, is indicated as treatment in chronic and refractory cases. However, the fear of postoperative incontinence leads many patients to seek less invasive options.
Recent studies are seeking assertive non-surgical alternatives, especially for those who have not achieved the desired results with laxatives or conventional ointments.
Clinical Research
Clinical research represents a stage of great importance for the advancement of modern medicine. Ethically and highly regulated, they are responsible for transforming scientific discoveries into real and accessible treatments, ensuring that each new option undergoes rigorous tests of efficacy, safety, and quality.
In the case of perianal fissure, clinical studies have played an important role in the development of less invasive and more comfortable alternatives than traditional surgeries.
The focus is to provide pain relief, truly effective healing, and complete preservation of anal function, avoiding complications like incontinence or prolonged discomfort.
What can a clinical study offer?
Participating in a clinical research study allows the patient to have free and supervised access to innovative therapies, overseen by specialist physicians and multidisciplinary teams.
The entire process follows international safety protocols, with approval from ethics committees and regulatory bodies that ensure the well-being and rights of volunteers.
Among the main advantages of joining a clinical study are:
Early access to treatments under evaluation and cutting-edge that are not yet available on the market.
Continuous and free medical follow-up, with included exams and consultations.
Supervised and monitored environment, ensuring safety at all stages.
Direct contribution to the advancement of science, helping others with the same condition.
Psychological and educational support, promoting understanding and peace of mind about the condition.
These studies are conducted with transparency, informed consent, and close monitoring, so that the participant knows about all stages and benefits of the study.
Perianal fissure: prevention and home care
Preventing perianal fissure is based on healthy bowel habits, proper hygiene, and stress management. A diet rich in fibers, adequate water intake, and regular physical activity significantly reduce risk, as they maintain balanced intestinal transit without constipation.
Moreover, being careful at the time of defecation is extremely important: delaying bowel movements or forcing stool passage increases the risk of microfissures, which can evolve into painful lesions that heal slowly.
Prolonged stress can also interfere with intestinal motility and promote constipation, creating a cycle that aggravates anorectal health. Taking care of diet, maintaining a proper sleep routine, and adopting relaxing practices strengthen the prevention of anal fissure.
How to prevent anal fissure

Before offering a list, it is important to explain that small routine changes have a significant impact on prevention. Anal fissure is often the result of poor bowel habits and lack of attention to digestive health, which makes the condition preventable.
Prevention should also include attention to early symptoms - such as burning, itching, or mild discomfort during defecation - which may indicate local irritation. In these cases, seeking medical guidance before the lesion worsens is the best way to avoid an acute fissure or the development of a chronic fissure.
Among the recommended preventive measures, we can list:
Increase fiber intake (fruits, vegetables, whole grains);
Drink 2 liters of water per day;
Avoid straining during bowel movements;
Engage in regular physical activity;
Maintain gentle anal hygiene.
These practices help to preserve the integrity of the anal mucosa and reduce the risk of recurrence. With consistent adoption of these habits, the body naturally adjusts, making intestinal transit smoother and reducing pressure exerted on the sphincter during defecation.
How to care for anal fissure at home?
Even after diagnosis, some home measures significantly aid recovery. Home care should always complement medical treatment and never replace it.
The patient should pay attention to thermal comfort and proper hygiene, as the anal region is highly sensitive and prone to irritation. Adopting simple habits, such as using neutral soaps and controlling sitting time, can improve local blood flow and reduce inflammation.
Patience is an important factor: even small fissures take weeks to fully heal. Some recommended care includes:
Warm sitz baths after defecation;
Avoid using dry toilet paper, preferring to wash the area with water after defecating or, if not possible, using neutral wet wipes;
Wear breathable and loose underwear;
Drink water regularly and consume fiber-rich foods, such as fruits and vegetables, to maintain good intestinal function.
With discipline and medical guidance, these actions help control symptoms and prevent complications. It is essential not to interrupt treatment before the recommended time and to maintain regular clinical follow-up, ensuring that the fissure heals properly and without leaving sequelae.
When to seek a doctor?
The presence of intense pain, persistent bleeding, or symptoms lasting more than four weeks requires specialized medical evaluation. Early diagnosis is important to prevent the fissure from becoming chronic and to avoid the need for surgical procedures.
Ignoring the signs can lead to worsening pain, the formation of spasms in the anal sphincter, and even local infection, resulting in abscesses or fistulas. Consulting a coloproctologist ensures a safe therapeutic plan, based on evidence and tailored to each patient's needs.
How to participate in a perianal fissure study?
Participating in a clinical study on perianal fissures is an opportunity to receive specialized medical follow-up, with free access to innovative therapies and constant support throughout the process.
The studies are conducted by certified research centers, supervised by ethics committees and health authorities, ensuring that each participant is treated with respect, safety, and absolute confidentiality.
By participating, you contribute not only to your own well-being but also to the advancement of science, helping to develop new therapeutic approaches for people suffering from the same condition.
If you experience intense pain while defecating, bleeding, burning, or fear of undergoing surgery, know that new possibilities are being studied right now - and your involvement can be part of this transformation.
Click the button below to participate in the study and receive a free assessment with the Synvia team.
______________________________________________________________________________________
REFERENCES:
MSD MANUAL – Anal fissure – Professional (specific page). Available at: https://www.msdmanuals.com/professional/gastrointestinal-disorders/anorectal-disorders/anal-fissure
MAYO CLINIC – Anal Fissure: Symptoms and causes. Available at: https://www.mayoclinic.org/diseases-conditions/anal-fissure/symptoms-causes/syc-20351424
CLEVELAND CLINIC – Anal Fissures. Available at: https://my.clevelandclinic.org/health/diseases/13177-anal-fissures
STATPEARLS / NCBI BOOKSHELF – Anal Fissure (overview / clinical pearls). Available at: https://www.ncbi.nlm.nih.gov/books/NBK549867/
PUBMED CENTRAL – GONZALEZ et al., Benign anorectal disease: hemorrhoids, fissures, and fistulas, 2019. Available at: https://www.ncbi.nlm.nih.gov/pmc/articles/PMC6928486/
AMERICAN SOCIETY OF COLON AND RECTAL SURGEONS (ASCRS) – Anal Fissure: patient information / guidelines. Available at: https://fascrs.org/patients/diseases-and-conditions/a-z/anal-fissure


